Hemochromatosis: Difference between revisions
imported>Thomas Simmons No edit summary |
imported>Thomas Simmons |
||
| Line 17: | Line 17: | ||
[[Armand Trousseau]], in an article on [[diabetes mellitus|diabetes]], first described the disease in 1865 but did not make the association with iron accumulation.<ref name=Trousseau_1865>{{cite journal | author = Trousseau A| title = Glycosurie, diabète sucré | journal = Clinique médicale de l'Hôtel-Dieu de Paris | year = 1865 | volume = 2| pages = 663–98 | url= }}</ref> [[Friedrich Daniel von Recklinghausen]] in 1890 linked the disease with iron accumulation.<ref>{{cite journal | author = von Recklinghausen FD | title = Hämochromatose | journal = Tageblatt der Naturforschenden Versammlung 1889 | year = 1890 | pages = 324 | url= }}</ref><ref>[http://www.whonamedit.com/doctor.cfm/1174.html Biography of Daniel von Recklinghausen]</ref> | [[Armand Trousseau]], in an article on [[diabetes mellitus|diabetes]], first described the disease in 1865 but did not make the association with iron accumulation.<ref name=Trousseau_1865>{{cite journal | author = Trousseau A| title = Glycosurie, diabète sucré | journal = Clinique médicale de l'Hôtel-Dieu de Paris | year = 1865 | volume = 2| pages = 663–98 | url= }}</ref> [[Friedrich Daniel von Recklinghausen]] in 1890 linked the disease with iron accumulation.<ref>{{cite journal | author = von Recklinghausen FD | title = Hämochromatose | journal = Tageblatt der Naturforschenden Versammlung 1889 | year = 1890 | pages = 324 | url= }}</ref><ref>[http://www.whonamedit.com/doctor.cfm/1174.html Biography of Daniel von Recklinghausen]</ref> | ||
==''' | =='''Synonyms for hemochromatosis'''== | ||
* | *Acquired hemochromatosis | ||
*Bronze diabetes | |||
* | |||
*Classical hemochromatosis | *Classical hemochromatosis | ||
*Genetic iron poisoning | *Genetic iron poisoning | ||
*Genetic hemochromatosis | *Genetic hemochromatosis | ||
*Hereditary hemochromatosis (HH or HHC) | |||
*Hepatic iron overload | |||
*Iron overload disease | |||
*Iron deposition disease | |||
*neonatal iron overload | |||
*neonatal hemochromatosis | |||
*Primary hemochromatosis | |||
*Secondary hemochromatosis | *Secondary hemochromatosis | ||
<ref>[http://www.nhlbi.nih.gov/health/dci/Diseases/hemo/hemo_othernames.html Other names for Hemochromatosis] National Institutes of Health</ref><ref>[http://www.emedicine.com/derm/topic878.htm Hemochromatosis</ref> | |||
<ref>[http://www.nhlbi.nih.gov/health/dci/Diseases/hemo/hemo_othernames.html Other names for Hemochromatosis] National Institutes of Health</ref> | |||
='''Types of Hemochromatosis'''= | ='''Types of Hemochromatosis'''= | ||
Revision as of 20:46, 22 March 2007
Template:DiseaseDisorder infobox
Haemochromatosis (UK spelling), or hemochromatosis (USA spelling) (pronunciation: he'-mo/kro-mah/to'-sis).
Hemochromatosis ('hemo' from the Greek for haima or blood, 'chroma' from the Greek chroma or color, and 'osis', denoting a morbid or abnormal process) is most commonly an hereditary disease (endogenous form) characterized by improper metabolisis of dietary iron which causes iron to accumulate in a number of body tissues,[1] eventually causing organ dysfunction. The less common exogenous form is caused by metabolic iron overload whch may occur in cases of chronic anemia, chronic liver disease and excessive iron supplementation (rare).
History
Armand Trousseau, in an article on diabetes, first described the disease in 1865 but did not make the association with iron accumulation.[2] Friedrich Daniel von Recklinghausen in 1890 linked the disease with iron accumulation.[3][4]
Synonyms for hemochromatosis
- Acquired hemochromatosis
- Bronze diabetes
- Classical hemochromatosis
- Genetic iron poisoning
- Genetic hemochromatosis
- Hereditary hemochromatosis (HH or HHC)
- Hepatic iron overload
- Iron overload disease
- Iron deposition disease
- neonatal iron overload
- neonatal hemochromatosis
- Primary hemochromatosis
- Secondary hemochromatosis
Types of Hemochromatosis
There exists two major types of hemochromatosis, hereditary (primary) hemochromatosis and acquired (secondary) hemochromatosis.[7]
Primary Hemochromatosis
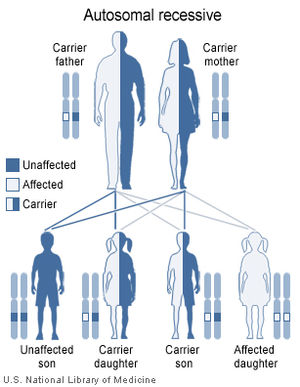
A genetic defect in the genes that control iron dietary absorption (HFE genes) is the cause of primary hemochromatosis. This is hereditary hemochromatosis (also known as classical hemochromatosis). The majority of hemochromatosis cases are primary. Primary hemochromatosis occurs with the inheritance of two copies of the abnormal HFE gene, one from each parent (i.e. are homogenous for the genetic defect).
Inheriting one abnormal HFE gene and one normal HFE gene (heterozygous for the genetic defect), results in a condition known as a hemochromatosis “carrier.” Carriers do not usually develop the disease, but they may pass the abnormal gene on to their children. About 1 in 10 people in the USA are believed to be carriers.
Other less common types of abnormal genes have also been linked to hemochromatosis.
Secondary Hemochromatosis
Secondary or acquired hemochromatosis is predominantly a result of other diseases or conditions causing iron overload. These include:
- Specific anemias (e.g. thalassemia or aplastic anemia);
- African iron overload, a combination of an inherited disorder and diet;
- Atransferrinemia and aceruloplasminemia, rare inherited diseases:
- Chronic liver disease (e.g. hepatitis, alcoholic liver disease, or nonalcoholic steatohepatitis - fatty hepatitis);
- High iron intake:
- Blood transfusions
- Iron intake (oral iron pills or injected iron)
- Long-term kidney dialysis
Signs and symptoms
Mimicry: Haemochromatosis is notoriously protean, i.e., it presents with symptoms that are often initially attributed to other diseases. In other words, the disease mimics other disease leading to mistaken diagnosis. It is also true that some people with the disease never actually show signs or suffer symptoms (i.e. is clinically silent).[8]
Symptoms: Symptoms may include [9][10][11]:
- Malaise
- Liver cirrhosis (with an increased risk of hepatocellular carcinoma, affecting up to a third of all homozygotes) - this is often preceded by a period of a painfully enlarged liver.
- Insulin resistance (often patients have already been diagnosed with diabetes mellitus type 2)
- Erectile dysfunction and hypogonadism
- Decreased libido
- Congestive heart failure, arrhythmias or pericarditis
- Arthritis of the hands (MCP and PIP joints), knee and shoulder joints
- Deafness[12]
- Dyskinesias, including Parkinsonian symptoms[13] [12] [14]
- Dysfunction of certain endocrine organs:
- Pancreatic gland
- Adrenal gland (leading to adrenal insufficiency)
- Parathyroid gland (leading to hypocalcaemia)
- Pituitary gland
- Testes or ovary (leading to hypogonadism)
- Pigmentation changes: A darkish colour to the skin (see pigmentation, hence its name Diabete bronze when it was first described by Armand Trousseau in 1865)
- Increased disease suceptibility: Increased susceptibility to disease may be caused by inhibition of phagocytosis, inhibition of intracellular killing of bacteria, and altered polymorphonuclear cell function. [15] The increased susceptibility to certain infectious diseases caused by:
- Vibrio vulnificus infections from eating seafood
- Listeria monocytogenes
- Yersinia enterocolica
- Salmonella enteritidis (serotype Typhymurium)
- Klebsiella pneumoniae
- Escherichia coli
- Rhizopus arrhizus
- Mucor species
Sex differences in diagnostic findings: Males are usually diagnosed after their forties, and women about a decade later, owing to regular iron loss by menstruation (which ceases in menopause),[16] but cases have been found in young children as well.
Diagnosis
Hemochromatosis is difficult to diagnose in the early stages. Early signs may mimic other diseases. Stiff joints and fatigue for example are common in haemochromatosis and other maladies.[17]
Lab Chemistry
Serum transferrin saturation: A first step is the measurement of transferrin, the protein which chemically binds to iron and carries it through the blood to the liver, spleen and bone marrow[18]. Measuring transferrin provides a measurement of iron in the blood. Saturation values of 45% are too high.[19]
Serum Ferritin: Ferritin, the protein which chemically binds to iron and stores it in the body. Measuring ferritin provides a measurement of iron in the whole body. Normal values for males are 12-300 ng/ml (nanograms per milliliter) and for female, 12-150 ng/ml. Low values indicate iron deficiency which may be attributed to a number of causes. Higher than normal also may indicate other causes including haemochromatosis.[20][21]
Additional lab testing: Other blood tests routinely performed: blood count, renal function, liver enzymes, electrolytes, glucose (and/or an oral glucose tolerance test (OGTT)).
Patient History: Based on the history, the doctor might consider specific tests to monitor organ dysfunction, such as an echocardiogram for heart failure.
Histopathology
Liver biopsy - Liver biopsies involve taking a sample of tissue from your liver, using a thin needle. The sample is then checked for the presence of iron as well as for evidence of liver damage (particularly cirrhosis: tissue scarring). Formerly, this was the only way to confirm a diagnosis of hemochromatosis but measures of transferrin and ferritin along with a history are considered better options in determining the presence of the malady. Risks of biopsy include bruising, bleeding and infection. Now, when a history and measures of transferrin or ferritin point to haemochromatosis, it is debatable whether a liver biopsy still needs to occur to quantify the amount of accumulated iron. [22]
Screening
Screening specifically means looking for a disease in people who have no symptoms. Diagnosis, on the other hand refers to testing people who have symptoms of a disease. Standard diagnostic measures for haemochromatosis, serum transferrin saturation and serum ferritin tests, aren't a part of routine medical testing. Screening for hemochromatosis is recommended if the patient has a parent, child or sibling with the disease, or have any of the following signs and symptoms: [23][24]
- Joint disease
- Severe fatigue
- Heart disease
- Elevated liver enzymes
- Impotence
- Diabetes
Genetic screening does not have any apparent advantages and treatment based on screening results are not demonstrably efficacious. Given that the malady is very rare in the general population, genetic carriers of the disease may never manifest the symptoms of the disease and the potential harm of the attendant surveillance, labeling, unnecessary invasive work-up, anxiety, and, potentially, unnecessary treatments outweigh the potential benefits. [25]
Epidemiology
Hemochromatosis is one of the most common inheritable genetic defects, especially in people of northern European extraction, with about 1 in 10 people carrying the defective gene. The prevalence of haemochromatosis varies in different populations. In Northern Europeans it is of the order of one in 400 persons. A study of 3,011 unrelated white Australians found that 14% were carriers and 0.5% had the genetic condition.[26]
Genetics
The gene that controls the amount of iron absorbed from food is called HFE. The HFE gene has two common mutations, C282Y and H63D.[27]
Inheriting just one of the C282Y mutations (heterozygous) makes a person a carrier who can pass this mutation onward. One mutation may lead to slightly excessive iron absorbtion but usually haemochromatosis does not develop.
In the United States, most people with haemochromatosis have inherited two copies of C282Y — one from each parent — and are homozygous for the trait. Mutations of the HFE gene account for 90% of the cases. This gene is closely linked to the HLA-A3 locus. Homozygosity for the C282Y mutation is the most significant, although hemochromatosis for the heterozygosity for C282Y/H63D mutations is very rare. Carriers of a single copy of either gene also have a very slight risk of haemochromatosis when other factors contribute, but are otherwise healthy.[28]
Other genes that cause haemochromatosis are the autosomal dominant SLC11A3/ferroportin 1 gene and TfR2 (transferrin receptor 2). They are much rarer than HFE-haemochromatosis.
Recently, a classification has been developed (with chromosome locations):
- Haemochromatosis type 1 (Online Mendelian Inheritance in Man, OMIM®. Johns Hopkins University, Baltimore, MD. MIM Number: 235200. World Wide Web URL: http://omim.org/.): "classical" HFE-haemochromatosis (6p21.3).
- Haemochromatosis type 2 (Online Mendelian Inheritance in Man, OMIM®. Johns Hopkins University, Baltimore, MD. MIM Number: 602390. World Wide Web URL: http://omim.org/.): juvenile haemochromatosis :
- Type 2A:(Online Mendelian Inheritance in Man, OMIM®. Johns Hopkins University, Baltimore, MD. MIM Number: 602390. World Wide Web URL: http://omim.org/.): mutations in hemojuvelin ("HJV", also known as HFE2)
- Type 2B (Online Mendelian Inheritance in Man, OMIM®. Johns Hopkins University, Baltimore, MD. MIM Number: 606464. World Wide Web URL: http://omim.org/.): mutation in hepcidin antimicrobial peptide (HAMP) or HFE2B (19q13)
- Haemochromatosis type 3 (Online Mendelian Inheritance in Man, OMIM®. Johns Hopkins University, Baltimore, MD. MIM Number: 604720. World Wide Web URL: http://omim.org/.): transferrin receptor-2 (TFR2 or HFE3, 7q22).
- Haemochromatosis type 4 (Online Mendelian Inheritance in Man, OMIM®. Johns Hopkins University, Baltimore, MD. MIM Number: 604653. World Wide Web URL: http://omim.org/.): autosomal dominant haemochromatosis (all others are recessive), ferroportin (SLC11A3) gene mutation (2q32).
Pathophysiology
People with the abnormal genes do not have the normal metabolic process to reduce their absorption of iron in response to increased iron levels in the body. Thus the iron stores of the body increase. As they increase the iron which is initially stored as ferritin starts to get stored as a breakdown product of ferritin called haemosiderin and this is toxic to tissue, probably at least partially by inducing Oxidative stress.[29]
Complications
Iron is stored in the liver, the pancreas and the heart. Long term effects of haemochromatosis on these organs can be very serious, even fatal when untreated. [30]
Cirrhosis: Permanent scarring of the liver. Along with other maladies like long-term alcoholism, haemochromatosis may have an adverse effect on the liver. The liver is a primary storage area for iron and will naturally accumulate excess iron. Over time the liver is likely to be damaged by iron overload. Cirrhosis itself may lead to additional and more serious complications, including bleeding from dilated veins in the esophagus and stomach (varices) and severe fluid retention in the abdomen (ascites). Toxins may accumulate in your blood and eventually affect mental functioning. This can lead to confusion or even coma (hepatic encephalopathy).
Liver cancer: Cirrhosis and haemochromatosis together will increase the risk of liver cancer. (Nearly one-third of people with haemochromatosis and cirrhosis eventually develop liver cancer.)
Diabetes: The pancreas which also stores iron is very important in the body’s mechanisms for sugar metabolism. Diabetes affects the way the body uses blood sugar (glucose). Diabetes is in turn the leading cause of new blindness in adults and may be involved in kidney failure and cardiovascular disease.
Congestive heart failure: If excess iron in the heart interferes with the its ability to circulate enough blood, a number of problems can occur including death. The condition may be reversible when haemochromatosis is treated and excess iron stores reduced.
Heart arrhythmias: Arrhythmia or abnormal heart rhythms can cause heart palpitations, chest pain and light-headedness and are occasionally life threatening. This condition can often be reversed with treatment for haemochromatosis.
Pigment changes: Deposits of iron in skin cells can turn skin a bronze or gray color.
Treatment
Early diagnosis is important because the late effects of iron accumulation can be wholly prevented by periodic phlebotomies (by venesection) comparable in volume to blood donations.[31] Treatment is initiated when ferritin levels reach 300 micrograms per litre (or 200 in nonpregnant premenopausal women).
Every 450-500 ml) of blood contains 200-250 milligrams of iron. Phlebotomy (or bloodletting) is usually done at a weekly interval until ferritin levels are less than 50 nanograms per millilitre. After that, 1-4 donations per year are usually needed to maintain iron balance.
Other parts of the treatment include:
- Treatment of organ damage (heart failure with diuretics and ACE inhibitor therapy).
- Limiting intake of alcoholic beverages, vitamin C (increases iron absorption in the gut), red meat (high in iron) and potential causes of food poisoning (shellfish, seafood).
- Increasing intake of substances that inhibit iron absorption, such as high-tannin tea, calcium, and foods containing oxalic and phytic acids (these must be consumed at the same time as the iron-containing foods in order to be effective.)
References
- ↑ Iron Overload and Hemochromatosis Centers for Disease Control and Prevention
- ↑ Trousseau A (1865). "Glycosurie, diabète sucré". Clinique médicale de l'Hôtel-Dieu de Paris 2: 663–98.
- ↑ von Recklinghausen FD (1890). "Hämochromatose". Tageblatt der Naturforschenden Versammlung 1889: 324.
- ↑ Biography of Daniel von Recklinghausen
- ↑ Other names for Hemochromatosis National Institutes of Health
- ↑ [http://www.emedicine.com/derm/topic878.htm Hemochromatosis
- ↑ What Causes Hemochromatosis? National Institutes of Health
- ↑ Hemochromatosis-Diagnosis National Digestive Diseases Information Clearinghouse, National Institutes of Health, U.S. Department of Health and Human Services
- ↑ Iron Overload and Hemochromatosis Centers for Disease Control and Prevention
- ↑ Hemochromatosis National Digestive Diseases Information Clearinghouse, National Institutes of Health, U.S. Department of Health and Human Services
- ↑ Hemochromatosis-Signs and Symptoms Mayo Foundation for Medical Education and Research (MFMER)
- ↑ 12.0 12.1 Jones H, Hedley-Whyte E (1983). "Idiopathic hemochromatosis (IHC): dementia and ataxia as presenting signs". Neurology 33 (11): 1479-83. PMID 6685241.
- ↑ Costello D, Walsh S, Harrington H, Walsh C (2004). "Concurrent hereditary haemochromatosis and idiopathic Parkinson's disease: a case report series". J Neurol Neurosurg Psychiatry 75 (4): 631-3. PMID 15026513.
- ↑ Nielsen J, Jensen L, Krabbe K (1995). "Hereditary haemochromatosis: a case of iron accumulation in the basal ganglia associated with a parkinsonian syndrome". J Neurol Neurosurg Psychiatry 59 (3): 318-21. PMID 7673967.
- ↑ Piagnerelli M, Rapotec A, Cotton F, Vincent JL. (2006). Iron Administration in the Critically III. Seminars in Hematology. Oct;43(4 Suppl 6):S23-7.
- ↑ Hemochromatosis Michelle Q. Bosworth (2002) Gale Encyclopedia of Genetic Disorders Part I. Healthline
- ↑ Screening and Diagnosis
- ↑ Transferrin and Iron Transport Physiology
- ↑ Screening and Diagnosis
- ↑ Screening and Diagnosis
- ↑ Ferritin Test Measuring iron in the body
- ↑ Screening and diagnosis Mayo Foundation for Medical Education and Research (MFMER) Retreived 18 March, 2007
- ↑ Screening and Diagnosis Mayo Foundation for Medical Education and Research (MFMER). Retreived 18 March, 2007
- ↑ Screening for Hereditary Hemochromatosis: Recommendations from the American College of Physicians Annals of Internal Medicine (2005) 4 October, Volume 143 Issue 7. (Page I-46). American College of Physicians. Retreived 18 March, 2007
- ↑ Screening for Hemochromatosis U.S. Preventive Services Task Force (2006). Summary of Screening Recommendations and Supporting Documents. Retreived 18 March, 2007
- ↑ Olynyk J, Cullen D, Aquilia S, Rossi E, Summerville L, Powell L (1999). "A population-based study of the clinical expression of the hemochromatosis gene". N Engl J Med 341 (10): 718-24. PMID 10471457.
- ↑ Hemochromatosis-Causes Mayo Foundation for Medical Education and Research (MFMER) Retreived March 12, 2007
- ↑ Hemochromatosis-Causes Mayo Foundation for Medical Education and Research (MFMER) Retreived March 12, 2007
- ↑ Shizukuda Y, Bolan C, Nguyen T, Botello G, Tripodi D, Yau Y, Waclawiw M, Leitman S, Rosing D (2007). "Oxidative stress in asymptomatic subjects with hereditary hemochromatosis". Am J Hematol 82 (3): 249-50. PMID 16955456.
- ↑ Haemochromatosis Complications
- ↑ Hemochromatosis - Treatment
See also
External links
- American Hemochromatosis Society
- Canadian Hemochromatosis Society
- Haemochromatosis page
- Causes of Haemochromatosis
- Iron Toxicity, What you don't know
- Andrews N (1999). "Disorders of iron metabolism". New England Journal of Medicine 341 (26): 1986-95. PMID 10607817.
link