Staphylococcus aureus: Difference between revisions
imported>Andrew QC Lee No edit summary |
imported>Meg Taylor No edit summary |
||
| (46 intermediate revisions by 7 users not shown) | |||
| Line 1: | Line 1: | ||
{{subpages}} | {{subpages}} | ||
{{Taxobox | {{Taxobox | ||
| color = violet | | color = violet | ||
| | | image = Staphylococcus-aureus.jpg | ||
| domain = [[Bacteria]] | | domain = [[Bacteria]] | ||
| phylum = [[Firmicutes]] | | phylum = [[Firmicutes]] | ||
| Line 14: | Line 12: | ||
| subdivision = ''Staphylococcus aureus'' | | subdivision = ''Staphylococcus aureus'' | ||
}} | }} | ||
'''''Staphylococcus aureus''''' is a [[Gram-positive]] spherical [[coccus]] that grows in a loose, irregular cluster resembling clusters of grapes. The cluster formation is due to the cell division occurring in three planes, with the daughter cell remaining in nearby. <ref name="isbn8125028080_page1">{{cite book |author=Paniker CKJ|chapter=|chapterurl=|editor= |title=Textbook of Microbiology |edition=7th|publisher=Orient Blackswan |location=Andhra Pradesh, India |year=2006 |pages= |isbn=8125028080 |page= |accessdate=|url=http://books.google.com/books?isbn=8125028080}}</ref> ''Staphylococcus aureus'' may also be found singly, in pairs and in short chains of three or four cells. The [[bacterium]] can never be found in long chains. They are non motile and non spore forming. On an ordinary medium, ''Staphylococcus aureus'' can grow within a temperature range of 10-42°C. The optimum pH ranges in between pH 7.4-7.6. The bacterium thrives best in an [[oxygen]] rich environment. ''S. aureus'' can grow on all common [[laboratory media]] such as milk, nutrient gelatin or agar. When grown on an [[agar|agar-based culture medium]] and incubated for 24 hours the colonies appear to be 2-4mm in diameter.<ref>[http://books.google.com/books?id=qCqBAYajT1EC&printsec=frontcover&dq=Textbook+of+Microbiology&sig=DR82H_pr4bXtR41QfPZ3mGXy8oE Textbook of Microbiology]</ref> The colonies appear circular, smooth, convex, shiny, and opaque.<ref>[http://books.google.com/books?id=qCqBAYajT1EC&printsec=frontcover&dq=Textbook+of+Microbiology&sig=DR82H_pr4bXtR41QfPZ3mGXy8oE Textbook of Microbiology]</ref> | |||
''Staphylococcus aureus'' was first observed in 1871 by von Recklinghausen but not isolated. Then in 1881 a surgeon by the name of Alexander Ogston documented two kinds of micrococci. The already known [[streptococci]], arranged in chains and the other cocci arranged in clusters. Ogston named the cocci cluster ''Staphylococci'' because “Staphyle” in Greek means "bunches of grapes" and “kokakos” meaning a "berry".<ref>[http://www.medicinenet.com/staph_infection/article.htm Medicinenet: Staphylococcus aureus]</ref> Unfortunately, Ogston did not provide a description of the genus and therefore it was not recognized. In 1884 Rosenbach successfully isolated and grew ''Staphylococcus aureus'' from pus. Rosenbach is credited with proposing the [[genus]] ''Staphylococcus'' and the species ''Staphylococcus aureus''.<ref>[http://books.google.com/books?id=qCqBAYajT1EC&printsec=frontcover&dq=Textbook+of+Microbiology&sig=DR82H_pr4bXtR41QfPZ3mGXy8oE Textbook of Microbiology]</ref> He kept the genus name ''Staphlococcus'' because the bacteria was similar to that studied by Ogston. Rosenbach proposed the [[nomenclature]] for ''Staphylococcus aureus'' based on the yellow pigmentation of the colony. | |||
''Staphylococcus aureus'' | |||
In recent years ''Staphylococcus aureus'' has become a serious health issue. The bacteria has built up a strong resistance to treatment. By unlocking the genome sequence, researchers could understand the nature of its resistance, [[virulence]], genetic flexibility, epidemiology and physiology. Comparing the genome sequence of ''S. aureus'' with the genomes of a less virulent form and [[nonpathogenic]] species could help researchers have a better understanding of the nature of ''Staphylococcal aureus'' infections. | |||
In recent years | |||
==Genome structure== | ==Genome structure== | ||
The ''Staphylococcus aureus'' genome contains about 2.800 to 2.903 million base pairs of DNA. The bacteria has about 2,600 genes in its chromosome. The first whole genome sequence of ''S. aureus'' strains were completed by shot-gun | The ''Staphylococcus aureus'' genome contains about 2.800 to 2.903 million [[base pairs]] of DNA. The bacteria has about 2,600 genes in its chromosome. The first whole genome sequence of ''S. aureus'' strains were completed by random shot-gun sequencing in 2001. ''S. aureus'' [[plasmids]] contains genes that encode resistance to [[antibiotic]]s, [[heavy metal]]s, or [[bacteriocide]]s.<ref>[http://www.medscape.com/viewarticle/565017_print Insights on Virulence and Antibiotic Resistance: A Review of the Accessory Genome of Staphylococcus aureus]</ref> Some virulence genes have been reported to be carried on plasmid, such as exfoliative toxin B and some superantigens.<ref>Yamaguchi T, Hayashi T, Takami H, et al. Complete nucleotide sequence of a Staphylococcus aureus exfoliative toxin B plasmid and identification of a novel ADPribosyltransferase, EDIN-C. Infect Immun. 2001;69(12):7760-7771.</ref> Approximately 75% of ''S. aureus'' genome comprises a core component of genes present in all of the strains.<ref>Lindsay JA, Holden MTG. Understanding the rise of the superbug: investigation of the evolution and genomic variation of Staphylococcus aureus. Funct Integr Genomics. 2006;6(3):186-201</ref> | ||
==Cell structure and metabolism== | ==Cell structure and metabolism== | ||
''Staphylococcus aureus'' cell wall contains a thick peptidoglycan layer and teichoic acid. The polysaccharide peptidoglycan in the cell wall gives the bacterium structure and rigidity and induces the release of cytokines. Teichoic acid is an antigenic component that aids adhesion of the cocci to the host cell surface. The bacterium contains no flagella. Some young cultures posses microscopically visible capsules. Many noncapsulated strains of ''S.aureus'' have small amounts of capsular material on the surface.<ref>[http://books.google.com/books?id=qCqBAYajT1EC&printsec=frontcover&dq=Textbook+of+Microbiology&sig=DR82H_pr4bXtR41QfPZ3mGXy8oE Textbook of Microbiology]</ref> | ''Staphylococcus aureus'' [[cell wall]] contains a thick [[peptidoglycan]] layer and [[teichoic acid]]. The [[polysaccharide]] peptidoglycan in the cell wall gives the bacterium structure and rigidity and induces the release of [[cytokines]]. Teichoic acid is an antigenic component that aids adhesion of the cocci to the host cell surface. The bacterium contains no flagella. Some young cultures posses microscopically visible capsules. Many noncapsulated strains of ''S.aureus'' have small amounts of capsular material on the surface.<ref>[http://books.google.com/books?id=qCqBAYajT1EC&printsec=frontcover&dq=Textbook+of+Microbiology&sig=DR82H_pr4bXtR41QfPZ3mGXy8oE Textbook of Microbiology]</ref> | ||
Staphylococci are [[facultative anaerobes]] that grow by [[aerobic respiration]] or by [[fermentation]] that yields [[lactic acid]]. ''S. aureus'' ferments sugars by producing acid but no gas. | Staphylococci are [[facultative anaerobes]] that grow by [[aerobic respiration]] or by [[fermentation]] that yields [[lactic acid]]. ''S. aureus'' ferments sugars by producing acid but no gas. | ||
Phagocytosis is a mechanism used by the host organism to combat a staphylococcal infections. ''S. aureus'' produces leukocidin, which cause the | [[Phagocytosis]] is a mechanism used by the host organism to combat a staphylococcal infections. ''S. aureus'' produces leukocidin, which cause the destruction of leukocytes allowing the bacteria to escape phagocytosis.<ref>Brock, Madigan, Martinko, Parker. ''Biology of Microorganisms'' New Jersey: Prentice Hall, 1994.</ref> Leukocidin is produced in skin lesions such as boils which results in cell destruction of white blood cells and is one of the factors responsible for pus formation. | ||
==Ecology== | ==Ecology== | ||
''Staphylococcus aureus'' is commonly found on the skin and in various mucous membranes of man and other animals. About 20-30% of healthy people in the United States are carriers of the bacteria.<ref>[http://www.medicinenet.com/staph_infection/article.htm Medicinenet: Staphylococcus aureus]</ref> These individuals are usually unaware that they are carriers of the bacteria and usually never get sick from it. In hospitals the percentage is higher because of more possible contact with infected cases | ''Staphylococcus aureus'' is commonly found on the skin and in various mucous membranes of man and other animals. About 20-30% of healthy people in the United States are carriers of the bacteria.<ref>[http://www.medicinenet.com/staph_infection/article.htm Medicinenet: Staphylococcus aureus]</ref> These individuals are usually unaware that they are carriers of the bacteria and usually never get sick from it. In hospitals the percentage is higher because of more possible contact with infected cases. | ||
==Pathology== | ==Pathology== | ||
[[Image:Furuncles_(boils)_.jpg]] | |||
Staphyolococcus aureus may cause furuncles (boils). | |||
The exfoliative (epidermolytic)toxin is responsible for staphylococcal scalded skin syndrome(SSSS). | |||
''Staphylococcus aureus'' is one of the most common pathogenic bacteria. The organism may cause disease through tissue invasion and toxin production. The bacteria could cause a wide range of infections both internally and externally. It may cause skin infections, bone infections, [[pneumonia]], food poisoning, Toxic shock syndrome, [[bacterial endocarditis]], life threatening bloodstream infections and other serious illnesses. | |||
'' | ''Staphyolococcus aureus'' may cause skin [[abscess]]es (boils) usually by entering the skin through a hair follicle or a cut. They may be red, swollen and painful, and sometimes have pus. They can turn into impetigo, which turns into a crust on the skin and usually common among newborns. The organism could also cause internal [[abscess]]es. | ||
In recent years ''Staphylococcus aureus'' has become one of the leading causes of [[cross infection]]s (hospital acquired infections). People prone to staphylococcal infections include newborns, drug users, breastfeeding women, and people with skin disorders, surgical incisions, a weakened immune system, or chronic diseases.<ref>[http://www.merck.com/mmhe/sec17/ch190/ch190r.html Merck: Staphylococcal Infections]</ref> | |||
Extracellular and cell associated factors may influence virulence. Cell surface proteins, extracellular enzymes and toxins are present on most strains of ''S. aureus'' and increases the species ability to act as a successful pathogen. | Extracellular and cell associated factors may influence virulence. Cell surface proteins, extracellular enzymes and toxins are present on most strains of ''S. aureus'' and increases the species ability to act as a successful pathogen. | ||
Protein A and clumping factors are both cell surface proteins. | Protein A and clumping factors are both cell surface proteins. [[Protein A]] induces [[platelet]] damage and hypersensitivity. The cocci clumps when introduced to human [[plasma]] because of this researchers use a coagulase test to help identify the bacterium. Some strains may not always test positive because they may be encapsulated. | ||
Coagulase, | [[Coagulase]], [[nuclease]]s, [[lipases]], [[hyaluronidase]] and protein receptors are all extracellular enzymes that play an important role in pathogenesis. The bacteria can convert fibrinogen to [[fibrin]], has a heat stable nuclease, produces lipid hydrolases which aids in infecting the skin, breaks down connective tissue, and possess receptors that facilitate adhesion to the host cell and tissue. | ||
Toxins such as alpha hemolysin, enterotoxin, toxic shock syndrome toxin(TSST), and exfoliative (epidermolytic)toxin produced by ''S. aureus'' may cause the bacerium to be more virulent. Alpha hemolysin is a protein that is inactivated at 70<sup>o</sup>C but activated at 100<sup>o</sup>C. It is toxic to macrophages, lysosomes, muscle tissues, renal cortex, and the circulatory system. Enterotoxin is also a superantigen responsible for causing food poisoning which may lead to nausea, vomiting, and diarrhea. Toxic shock syndrome toxin is a | Toxins such as alpha hemolysin, [[enterotoxin]], toxic shock syndrome toxin(TSST), and exfoliative (epidermolytic)toxin produced by ''S. aureus'' may cause the bacerium to be more virulent. Alpha hemolysin is a protein that is inactivated at 70<sup>o</sup>C but activated at 100<sup>o</sup>C. It is toxic to macrophages, lysosomes, muscle tissues, renal cortex, and the circulatory system. Enterotoxin is also a superantigen responsible for causing food poisoning which may lead to nausea, vomiting, and diarrhea. Toxic shock syndrome toxin is a [[super antigen]] as well and causes toxic shock syndrome in the infected host. It may prove to be a potentially fatal multi system disease. The infected host can experience a fever, hypotension, myalgia, vomiting, diarrhea and mucosal hyperemia. The exfoliative (epidermolytic)toxin is responsible for [[staphylococcal scalded skin syndrome]](SSSS). It is an exfoliative skin disease which causes the outer layer of the epidermis to be separated from the underlying tissues. Symptoms associated with the disease are a fever, malaise and irritability following an upper respiratory infection. | ||
''Staphylococcus aureus'' has a high incidence of drug resistance with methicillin-resistant strains resistant to ß-lactams and most other antibiotics. Infections are enhanced in the presence of foreign materials inside the body such as tampons, surgical packing or intravenous catheters | ''Staphylococcus aureus'' has a high incidence of drug resistance with methicillin-resistant strains resistant to ß-lactams and most other antibiotics. Infections are enhanced in the presence of foreign materials inside the body such as tampons, surgical packing or intravenous catheters. | ||
==Application to Biotechnology== | ==Application to Biotechnology== | ||
In an [[anaerobic]] environment ''Staphylococcus aureus'' can reduce mannitol to lactic acid, which differentiates it from other species of staphylococci. The bacterium is the only coagulase positive and ß-hemolytic staphylococcus. When grown on a nutrient agar containing phenolphthalein diphosphate the bacterium produces phosphatase. When ammonia vapor is introduced to the culture, the colonies assume a bright pink color due to the presence of free [[phenolphthalein]]. Researchers use this test to distinguish between ''Staphylococcus aureus'' from ''S. epidermidis''. | |||
''S. aureus'' is coagulase positive, ferments mannite, produce clear hemolysis on blood agar, liquefy gelatin, produces phosphatase, in a medium containing potassium it reduce tellurite to form black colonies and it produce thermostable nucleases. | |||
==Current Research== | ==Current Research== | ||
{{seealso|Cross infection}} | |||
There has always been a need for universal screening at hospitals for methicillin-resistant ''Staphylococcus aureus'' (MRSA) at time of admission of patients.<ref>{{citation | |||
| author = Harbarth S, Frankhauser C, Schrenzel J, Christenson J, Gervaz P, Bandiera-Clerc C, Renzi G, Vernaz N, Sax H, Pittet | |||
| title = Universal screening for methicillin-resistant Staphylococcus aureus at hospital admission and nosocomial infection in surgical patients | |||
| year = 2008 | journal = JAMA | url = http://www.galenicom.com/medline/printarticle/18334690 Galenicom.com]] | |||
}}</ref> A study was conducted from July 2004 to May 2006 to demonstrate the effect of early detection of MRSA infection rates in surgical patients. There were about 21, 754 patients involved in this study. The study compared rapid screening on admission plus standard infection control measure vs. standard infection control alone. The study showed that 94% of patients were screened at time of admission to the hospital. The screening identified 5.1% of the patients were MRSA positive and more that half of the 5.1% was unaware that they were carriers. During the rapid screening period 93 patients developed nosocomial MRSA infections and only 73 patients during the control period. The study revealed that universal screening for methicillin-resistant ''Staphylococcus aureus'' did not reduce nosocomial MRSA infections in surgical patients. <ref>{{citation | |||
| author = Patricia M. Mertz; Tatiana C. P. Cardenas; Richard V. Snyder; Megan A. Kinney; Stephen C. Davis; Lisa R. W. Plano | |||
| year = 2007 | |||
| title = Staphylococcus aureus Virulence Factors Associated With Infected Skin Lesions | |||
Influence on the Local Immune Response | |||
| journal = Arch Dermatol| volume = 143| url =http://archderm.ama-assn.org/cgi/content/abstract/143/10/1259}}</ref> | |||
The study examined ''Staphylococcus aureus'' strains from skin lesions for their potential to produce immune system- modulating toxins and to connect it to the number of white blood cells found in the infected skin lesions. There were 84 isolated bacterial chromosomal DNA obtained. They were categorized into two groups, those that correlated with a low white blood cell count and those with a high white blood cell count. The study indicated that there were a higher number of bacteria capable of producing exfoliative toxins A or B and Panton-Valentine leukocidin without taking into account the number of white blood cells. The research revealed that the ''S. aureus'' associated with a low number of white blood cells produced exfoliative toxins A or B. ''S. aureus'' associated with a high number of white blood cells produced toxins such as Panton-Valentine leukocidin and toxic shock syndrome toxin. The infected skin lesions appeared no different from each other. | |||
George Liu, Anthony Essex, John Buchanan, Vivekanand Datta, Hal Hoffman, John Bastian, Joshua Fierer and Victor Nizet.(2005) Staphylococcus aureus golden pigment impairs neutrophil killing and promotes virulence through its antioxidant activity. The Journal of Experimental Medicine, 202. Retrieved April 12, 2008 from [[http://www.jem.org/cgi/reprint/202/2/209.pdf The Journal of Experimental Medicine]] | |||
The research conducted demonstrated that the golden pigmentation of ''Staphylococcus aureus'' is a virulence factor and could potentially to lead antimicrobial therapy. An ''S. aureus'' mutant was created with a disrupted carotenoid biosynthesis pathway. The pigment proved to have antioxidant properties. The study showed that a mutant strain missing the carotenoid coating was less pathogenic making it more vulnerable to free radicls. When the carotenoid biosynthesis pathway is inhibited there is an increase oxidant sensitivity. The ''S. aureus'' carotenoid play an important role in its resistance to neutrophil mediated killing. The inhibition of the carotenoid biosynthesis pathway may lead to a therapeutic approach to the treatment of ''Staphylococcus aureus'' infections. | |||
==Methicillin-resistant staphylococcus aureus== | ==Methicillin-resistant staphylococcus aureus== | ||
Methicillin-resistant staphylococcus aureus (MRSA) is a strain of ''Staphylococcus aureus'' that is resistant to commonly used [[antibiotic]]s such as methicillin. MRSA emerged in the early 1960's. MRSA is predominantly a nosocomial pathogen causing hospital | {{main|Methicillin resistant Staphylococcus aureus}} | ||
Methicillin-resistant staphylococcus aureus (MRSA) is a strain of ''Staphylococcus aureus'' that is resistant to commonly used [[antibiotic]]s such as methicillin. MRSA emerged in the early 1960's. MRSA is predominantly a nosocomial pathogen causing hospital acquired infections as well as community acquired infections. Currently available statistics from the Kaiser foundation in 2007 indicate that about 1.2 million hospitalized patients have MRSA, and the mortality rate is estimated to be between 4%-10%.<ref>{{citation | |||
| journal= Medicinenet | |||
| url = http://www.medicinenet.com/mrsa_infection/article.htm | |||
| title = MRSA Infection}}</ref> | |||
MRSA may be more virulent than other staphylococcus aureus due to carrying the gene for Panton-Valentine leucocidin (PVL). <ref name="pmid17846141">{{cite journal | |||
|author=Rajendran PM, Young D, Maurer T, ''et al'' | |||
|title=Randomized, Double-Blind, Placebo-Controlled Trial of Cephalexin for Treatment of Uncomplicated Skin Abscesses in a Population at Risk for Community-Acquired Methicillin-Resistant Staphylococcus aureus Infection | |||
|journal=Antimicrob. Agents Chemother. | |||
|volume=51 | |||
|issue=11 | |||
|pages=4044–8 | |||
|year=2007 | |||
|pmid=17846141 | |||
|doi=10.1128/AAC.00377-07}}</ref> | |||
==References== | ==References== | ||
{{reflist|2}} | |||
Latest revision as of 21:23, 15 December 2013
| Staphylococcus aureus | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| File:Staphylococcus-aureus.jpg | ||||||||||||
| Scientific classification | ||||||||||||
| ||||||||||||
| Species | ||||||||||||
|
Staphylococcus aureus |
Staphylococcus aureus is a Gram-positive spherical coccus that grows in a loose, irregular cluster resembling clusters of grapes. The cluster formation is due to the cell division occurring in three planes, with the daughter cell remaining in nearby. [1] Staphylococcus aureus may also be found singly, in pairs and in short chains of three or four cells. The bacterium can never be found in long chains. They are non motile and non spore forming. On an ordinary medium, Staphylococcus aureus can grow within a temperature range of 10-42°C. The optimum pH ranges in between pH 7.4-7.6. The bacterium thrives best in an oxygen rich environment. S. aureus can grow on all common laboratory media such as milk, nutrient gelatin or agar. When grown on an agar-based culture medium and incubated for 24 hours the colonies appear to be 2-4mm in diameter.[2] The colonies appear circular, smooth, convex, shiny, and opaque.[3]
Staphylococcus aureus was first observed in 1871 by von Recklinghausen but not isolated. Then in 1881 a surgeon by the name of Alexander Ogston documented two kinds of micrococci. The already known streptococci, arranged in chains and the other cocci arranged in clusters. Ogston named the cocci cluster Staphylococci because “Staphyle” in Greek means "bunches of grapes" and “kokakos” meaning a "berry".[4] Unfortunately, Ogston did not provide a description of the genus and therefore it was not recognized. In 1884 Rosenbach successfully isolated and grew Staphylococcus aureus from pus. Rosenbach is credited with proposing the genus Staphylococcus and the species Staphylococcus aureus.[5] He kept the genus name Staphlococcus because the bacteria was similar to that studied by Ogston. Rosenbach proposed the nomenclature for Staphylococcus aureus based on the yellow pigmentation of the colony.
In recent years Staphylococcus aureus has become a serious health issue. The bacteria has built up a strong resistance to treatment. By unlocking the genome sequence, researchers could understand the nature of its resistance, virulence, genetic flexibility, epidemiology and physiology. Comparing the genome sequence of S. aureus with the genomes of a less virulent form and nonpathogenic species could help researchers have a better understanding of the nature of Staphylococcal aureus infections.
Genome structure
The Staphylococcus aureus genome contains about 2.800 to 2.903 million base pairs of DNA. The bacteria has about 2,600 genes in its chromosome. The first whole genome sequence of S. aureus strains were completed by random shot-gun sequencing in 2001. S. aureus plasmids contains genes that encode resistance to antibiotics, heavy metals, or bacteriocides.[6] Some virulence genes have been reported to be carried on plasmid, such as exfoliative toxin B and some superantigens.[7] Approximately 75% of S. aureus genome comprises a core component of genes present in all of the strains.[8]
Cell structure and metabolism
Staphylococcus aureus cell wall contains a thick peptidoglycan layer and teichoic acid. The polysaccharide peptidoglycan in the cell wall gives the bacterium structure and rigidity and induces the release of cytokines. Teichoic acid is an antigenic component that aids adhesion of the cocci to the host cell surface. The bacterium contains no flagella. Some young cultures posses microscopically visible capsules. Many noncapsulated strains of S.aureus have small amounts of capsular material on the surface.[9]
Staphylococci are facultative anaerobes that grow by aerobic respiration or by fermentation that yields lactic acid. S. aureus ferments sugars by producing acid but no gas.
Phagocytosis is a mechanism used by the host organism to combat a staphylococcal infections. S. aureus produces leukocidin, which cause the destruction of leukocytes allowing the bacteria to escape phagocytosis.[10] Leukocidin is produced in skin lesions such as boils which results in cell destruction of white blood cells and is one of the factors responsible for pus formation.
Ecology
Staphylococcus aureus is commonly found on the skin and in various mucous membranes of man and other animals. About 20-30% of healthy people in the United States are carriers of the bacteria.[11] These individuals are usually unaware that they are carriers of the bacteria and usually never get sick from it. In hospitals the percentage is higher because of more possible contact with infected cases.
Pathology
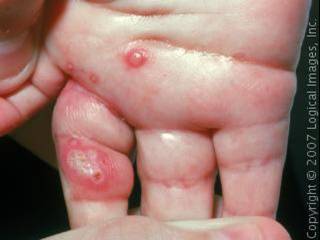 Staphyolococcus aureus may cause furuncles (boils).
The exfoliative (epidermolytic)toxin is responsible for staphylococcal scalded skin syndrome(SSSS).
Staphyolococcus aureus may cause furuncles (boils).
The exfoliative (epidermolytic)toxin is responsible for staphylococcal scalded skin syndrome(SSSS).
Staphylococcus aureus is one of the most common pathogenic bacteria. The organism may cause disease through tissue invasion and toxin production. The bacteria could cause a wide range of infections both internally and externally. It may cause skin infections, bone infections, pneumonia, food poisoning, Toxic shock syndrome, bacterial endocarditis, life threatening bloodstream infections and other serious illnesses.
Staphyolococcus aureus may cause skin abscesses (boils) usually by entering the skin through a hair follicle or a cut. They may be red, swollen and painful, and sometimes have pus. They can turn into impetigo, which turns into a crust on the skin and usually common among newborns. The organism could also cause internal abscesses.
In recent years Staphylococcus aureus has become one of the leading causes of cross infections (hospital acquired infections). People prone to staphylococcal infections include newborns, drug users, breastfeeding women, and people with skin disorders, surgical incisions, a weakened immune system, or chronic diseases.[12]
Extracellular and cell associated factors may influence virulence. Cell surface proteins, extracellular enzymes and toxins are present on most strains of S. aureus and increases the species ability to act as a successful pathogen.
Protein A and clumping factors are both cell surface proteins. Protein A induces platelet damage and hypersensitivity. The cocci clumps when introduced to human plasma because of this researchers use a coagulase test to help identify the bacterium. Some strains may not always test positive because they may be encapsulated.
Coagulase, nucleases, lipases, hyaluronidase and protein receptors are all extracellular enzymes that play an important role in pathogenesis. The bacteria can convert fibrinogen to fibrin, has a heat stable nuclease, produces lipid hydrolases which aids in infecting the skin, breaks down connective tissue, and possess receptors that facilitate adhesion to the host cell and tissue.
Toxins such as alpha hemolysin, enterotoxin, toxic shock syndrome toxin(TSST), and exfoliative (epidermolytic)toxin produced by S. aureus may cause the bacerium to be more virulent. Alpha hemolysin is a protein that is inactivated at 70oC but activated at 100oC. It is toxic to macrophages, lysosomes, muscle tissues, renal cortex, and the circulatory system. Enterotoxin is also a superantigen responsible for causing food poisoning which may lead to nausea, vomiting, and diarrhea. Toxic shock syndrome toxin is a super antigen as well and causes toxic shock syndrome in the infected host. It may prove to be a potentially fatal multi system disease. The infected host can experience a fever, hypotension, myalgia, vomiting, diarrhea and mucosal hyperemia. The exfoliative (epidermolytic)toxin is responsible for staphylococcal scalded skin syndrome(SSSS). It is an exfoliative skin disease which causes the outer layer of the epidermis to be separated from the underlying tissues. Symptoms associated with the disease are a fever, malaise and irritability following an upper respiratory infection.
Staphylococcus aureus has a high incidence of drug resistance with methicillin-resistant strains resistant to ß-lactams and most other antibiotics. Infections are enhanced in the presence of foreign materials inside the body such as tampons, surgical packing or intravenous catheters.
Application to Biotechnology
In an anaerobic environment Staphylococcus aureus can reduce mannitol to lactic acid, which differentiates it from other species of staphylococci. The bacterium is the only coagulase positive and ß-hemolytic staphylococcus. When grown on a nutrient agar containing phenolphthalein diphosphate the bacterium produces phosphatase. When ammonia vapor is introduced to the culture, the colonies assume a bright pink color due to the presence of free phenolphthalein. Researchers use this test to distinguish between Staphylococcus aureus from S. epidermidis.
S. aureus is coagulase positive, ferments mannite, produce clear hemolysis on blood agar, liquefy gelatin, produces phosphatase, in a medium containing potassium it reduce tellurite to form black colonies and it produce thermostable nucleases.
Current Research
- See also: Cross infection
There has always been a need for universal screening at hospitals for methicillin-resistant Staphylococcus aureus (MRSA) at time of admission of patients.[13] A study was conducted from July 2004 to May 2006 to demonstrate the effect of early detection of MRSA infection rates in surgical patients. There were about 21, 754 patients involved in this study. The study compared rapid screening on admission plus standard infection control measure vs. standard infection control alone. The study showed that 94% of patients were screened at time of admission to the hospital. The screening identified 5.1% of the patients were MRSA positive and more that half of the 5.1% was unaware that they were carriers. During the rapid screening period 93 patients developed nosocomial MRSA infections and only 73 patients during the control period. The study revealed that universal screening for methicillin-resistant Staphylococcus aureus did not reduce nosocomial MRSA infections in surgical patients. [14]
The study examined Staphylococcus aureus strains from skin lesions for their potential to produce immune system- modulating toxins and to connect it to the number of white blood cells found in the infected skin lesions. There were 84 isolated bacterial chromosomal DNA obtained. They were categorized into two groups, those that correlated with a low white blood cell count and those with a high white blood cell count. The study indicated that there were a higher number of bacteria capable of producing exfoliative toxins A or B and Panton-Valentine leukocidin without taking into account the number of white blood cells. The research revealed that the S. aureus associated with a low number of white blood cells produced exfoliative toxins A or B. S. aureus associated with a high number of white blood cells produced toxins such as Panton-Valentine leukocidin and toxic shock syndrome toxin. The infected skin lesions appeared no different from each other.
George Liu, Anthony Essex, John Buchanan, Vivekanand Datta, Hal Hoffman, John Bastian, Joshua Fierer and Victor Nizet.(2005) Staphylococcus aureus golden pigment impairs neutrophil killing and promotes virulence through its antioxidant activity. The Journal of Experimental Medicine, 202. Retrieved April 12, 2008 from [The Journal of Experimental Medicine]
The research conducted demonstrated that the golden pigmentation of Staphylococcus aureus is a virulence factor and could potentially to lead antimicrobial therapy. An S. aureus mutant was created with a disrupted carotenoid biosynthesis pathway. The pigment proved to have antioxidant properties. The study showed that a mutant strain missing the carotenoid coating was less pathogenic making it more vulnerable to free radicls. When the carotenoid biosynthesis pathway is inhibited there is an increase oxidant sensitivity. The S. aureus carotenoid play an important role in its resistance to neutrophil mediated killing. The inhibition of the carotenoid biosynthesis pathway may lead to a therapeutic approach to the treatment of Staphylococcus aureus infections.
Methicillin-resistant staphylococcus aureus
Methicillin-resistant staphylococcus aureus (MRSA) is a strain of Staphylococcus aureus that is resistant to commonly used antibiotics such as methicillin. MRSA emerged in the early 1960's. MRSA is predominantly a nosocomial pathogen causing hospital acquired infections as well as community acquired infections. Currently available statistics from the Kaiser foundation in 2007 indicate that about 1.2 million hospitalized patients have MRSA, and the mortality rate is estimated to be between 4%-10%.[15]
MRSA may be more virulent than other staphylococcus aureus due to carrying the gene for Panton-Valentine leucocidin (PVL). [16]
References
- ↑ Paniker CKJ (2006). Textbook of Microbiology, 7th. Andhra Pradesh, India: Orient Blackswan. ISBN 8125028080.
- ↑ Textbook of Microbiology
- ↑ Textbook of Microbiology
- ↑ Medicinenet: Staphylococcus aureus
- ↑ Textbook of Microbiology
- ↑ Insights on Virulence and Antibiotic Resistance: A Review of the Accessory Genome of Staphylococcus aureus
- ↑ Yamaguchi T, Hayashi T, Takami H, et al. Complete nucleotide sequence of a Staphylococcus aureus exfoliative toxin B plasmid and identification of a novel ADPribosyltransferase, EDIN-C. Infect Immun. 2001;69(12):7760-7771.
- ↑ Lindsay JA, Holden MTG. Understanding the rise of the superbug: investigation of the evolution and genomic variation of Staphylococcus aureus. Funct Integr Genomics. 2006;6(3):186-201
- ↑ Textbook of Microbiology
- ↑ Brock, Madigan, Martinko, Parker. Biology of Microorganisms New Jersey: Prentice Hall, 1994.
- ↑ Medicinenet: Staphylococcus aureus
- ↑ Merck: Staphylococcal Infections
- ↑ Harbarth S, Frankhauser C, Schrenzel J, Christenson J, Gervaz P, Bandiera-Clerc C, Renzi G, Vernaz N, Sax H, Pittet (2008), "Galenicom.com] Universal screening for methicillin-resistant Staphylococcus aureus at hospital admission and nosocomial infection in surgical patients]", JAMA
- ↑ Patricia M. Mertz; Tatiana C. P. Cardenas; Richard V. Snyder; Megan A. Kinney; Stephen C. Davis; Lisa R. W. Plano (2007), "[http://archderm.ama-assn.org/cgi/content/abstract/143/10/1259 Staphylococcus aureus Virulence Factors Associated With Infected Skin Lesions Influence on the Local Immune Response]", Arch Dermatol 143
- ↑ "MRSA Infection", Medicinenet
- ↑ Rajendran PM, Young D, Maurer T, et al (2007). "Randomized, Double-Blind, Placebo-Controlled Trial of Cephalexin for Treatment of Uncomplicated Skin Abscesses in a Population at Risk for Community-Acquired Methicillin-Resistant Staphylococcus aureus Infection". Antimicrob. Agents Chemother. 51 (11): 4044–8. DOI:10.1128/AAC.00377-07. PMID 17846141. Research Blogging.